Abstract
Background
Seizures are common after intracerebral hemorrhage (ICH) but their impact on outcome is uncertain and prophylactic anti-convulsant use is controversial. We hypothesized that seizures would not increase the risk of in-hospital mortality in a large administrative database.
Methods
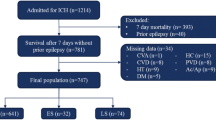
The study population included patients in the 2006 Nationwide Inpatient Sample over the age of 18 with a principal diagnosis of ICH (ICD9 = 431). Subjects with a secondary diagnosis of aneurysm, arterio-venous malformation, brain tumor, or traumatic brain injury were excluded. Seizures were defined by ICD9 codes (345.0x–345.5x, 345.7x–345.9x, 780.39). Logistic regression was used to quantify the relationship between seizures and in-hospital mortality. Pre-specified subgroups included age strata, length of stay, and invasive procedures.
Results
13,033 subjects met all eligibility criteria, of which 1,430 (11.0 %) had a secondary diagnosis of seizure. Subjects with seizure were younger (64 vs. 70 years, p < 0.001), more likely to get craniectomy (2.1 vs. 1.2 %, p = 0.006), ventriculostomy (8.5 vs. 6.0 %, p < 0.001), intubation (32.2 vs. 25.9 %, p < 0.001), and tracheostomy (6.4 vs. 4.2 %, p < 0.001). Seizure patients had lower in-hospital mortality (24.3 vs. 28.0 %, p = 0.003). In a multivariable model incorporating patient and hospital level variables, seizures were associated with reduced odds of in-hospital death (OR = 0.62, 95 % CI 0.52–0.75).
Conclusions
A secondary diagnosis of seizure after ICH was not associated with increased in-hospital death overall or in any of the pre-specified subgroups; however, there may be residual confounding by severity. These findings do not support a need for routine prophylactic anti-epileptic drug use after ICH.

Similar content being viewed by others
References
Berger AR, Lipton RB, Lesse ML, Lantos G, Portenoy RK. Early seizures following intracerebral hemorrhage: implications for therapy. Neurology. 1988;38:1363–5.
Bladin CF, Alexandrov AV, Bellavance A, et al. Seizures after stroke: a prospective multicenter study. Arch Neurol. 2000;57:1617–22.
Passero S, Rocchi R, Rossi S, Ulivelli M, Vatti G. Seizures after spontaneous supratentorial intracerebral hemorrhage. Epilepsia. 2002;43:1175–80.
Szaflarski JP, Rackley AY, Kleindorfer DO, et al. Incidence of seizures in the acute phase of stroke: a population-based study. Epilepsia. 2008;49:974–81.
Labovitz DL, Allen Hauser W, Sacco RL. Prevalence and predictors of early seizure and status epilepticus after first stroke. Neurology. 2001;57:200–6.
Kilpatrick CJ, Davis SM, Tress BM, Rossiter SC, Hopper JL, Vandendriesen ML. Epileptic seizures in acute stroke. Arch Neurol. 1990;47:157–60.
Messe SR, Sansing LH, Cucchiara BL, Herman ST, Lyden PD, Kasner SE. Prophylactic antiepileptic drug use is associated with poor outcome following ICH. Neurocrit Care. 2009;11(1):38–44.
Naidech AM, Garg RK, Liebling S, et al. Anticonvulsant use and outcomes after intracerebral hemorrhage. Stroke. 2009;40:3810–5.
Reddig RT, Nixdorf KE, Jensen MB. The prophylactic use of an antiepileptic drug in intracerebral hemorrhage. Clin Neurol Neurosurg. 2011;113:895–7.
Gilad R, Boaz M, Dabby R, Sadeh M, Lampl Y. Are post intracerebral hemorrhage seizures prevented by anti-epileptic treatment? Epilepsy Res. 2011;95:227–31.
Taylor S, Heinrichs RJ, Janzen JM, Ehtisham A. Levetiracetam is associated with improved cognitive outcome for patients with intracranial hemorrhage. Neurocritical care. 2011;15:80–4.
Morgenstern LB, Hemphill JC 3rd, Anderson C, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2010;41:2108–29.
Overview of the Nationwide Inpatient Sample (NIS). Healthcare Cost and Utilization Project. http://www.hcup-us.ahrq.gov/nisoverview.jsp (2011). Accessed 26 Nov 2011.
Kokotailo RA, Hill MD. Coding of stroke and stroke risk factors using international classification of diseases, revisions 9 and 10. Stroke. 2005;36:1776–81.
Tirschwell DL, Longstreth WT Jr. Validating administrative data in stroke research. Stroke. 2002;33:2465–70.
Jette N, Reid AY, Quan H, Hill MD, Wiebe S. How accurate is ICD coding for epilepsy? Epilepsia. 2010;51:62–9.
Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27.
Averill RFGN, Muldoon J, Steinbeck BA, Grant TM. A closer look at all-patient refined DRGs. J AHIMA. 2002;73:46–50.
Arboix A, Garcia-Eroles L, Massons JB, Oliveres M, Comes E. Predictive factors of early seizures after acute cerebrovascular disease. Stroke. 1997;28:1590–4.
Burneo JG, Fang J, Saposnik G. Impact of seizures on morbidity and mortality after stroke: a Canadian multi-centre cohort study. Eur J Neurol. 2010;17:52–8.
Reith J, Jorgensen HS, Nakayama H, Raaschou HO, Olsen TS. Seizures in acute stroke: predictors and prognostic significance. The Copenhagen stroke study. Stroke. 1997;28:1585–9.
De Herdt V, Dumont F, Henon H, et al. Early seizures in intracerebral hemorrhage: incidence, associated factors, and outcome. Neurology. 2011;77:1794–800.
Leira R, Davalos A, Silva Y, et al. Early neurologic deterioration in intracerebral hemorrhage: predictors and associated factors. Neurology. 2004;63:461–7.
Battey TW, Falcone GJ, Ayres AM, et al. Confounding by indication in retrospective studies of intracerebral hemorrhage: antiepileptic treatment and mortality. Neurocrit Care. 2012.
Vespa PM, O’Phelan K, Shah M, et al. Acute seizures after intracerebral hemorrhage: a factor in progressive midline shift and outcome. Neurology. 2003;60:1441–6.
Claassen J, Jette N, Chum F, et al. Electrographic seizures and periodic discharges after intracerebral hemorrhage. Neurology. 2007;69:1356–65.
Hemphill JC 3rd, Bonovich DC, Besmertis L, Manley GT, Johnston SC. The ICH score: a simple, reliable grading scale for intracerebral hemorrhage. Stroke. 2001;32:891–7.
Castellanos M, Leira R, Tejada J, Gil-Peralta A, Davalos A, Castillo J. Predictors of good outcome in medium to large spontaneous supratentorial intracerebral haemorrhages. J Neurol Neurosurg Psychiatry. 2005;76:691–5.
Conflict of interest
Dr. Mullen, Dr. Messé and Dr. Kasner have no relevant disclosures to report.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mullen, M.T., Kasner, S.E. & Messé, S.R. Seizures Do Not Increase In-Hospital Mortality After Intracerebral Hemorrhage in the Nationwide Inpatient Sample. Neurocrit Care 19, 19–24 (2013). https://doi.org/10.1007/s12028-012-9791-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-012-9791-0